On this page:
- What is spasmodic dysphonia?
- What are the types of spasmodic dysphonia?
- What causes spasmodic dysphonia?
- How is spasmodic dysphonia diagnosed?
- What treatment is available for spasmodic dysphonia?
- What research does the NIDCD support on spasmodic dysphonia?
- Where can I find more information on spasmodic dysphonia?
What is spasmodic dysphonia?
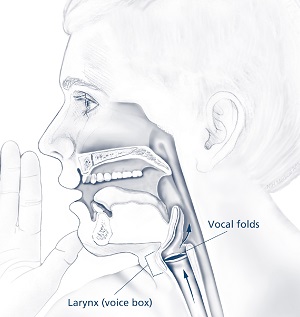
Parts of the throat involved in spasmodic dysphonia.
Source: NIH/NIDCD
Spasmodic dysphonia, or laryngeal dystonia, is a disorder affecting the voice muscles in the larynx, also called the voice box. When you speak, air from your lungs is pushed between two elastic structures—called vocal folds—causing them to vibrate and produce your voice. In spasmodic dysphonia, the muscles inside the vocal folds spasm (make sudden, involuntary movements), interfering with vocal fold vibrations. Spasmodic dysphonia may occur along with other forms of dystonia that cause repeated spasms in other parts of the body, including the eyes, face, jaw, lips, tongue, neck, arms, or legs.
Spasmodic dysphonia causes voice breaks during speaking and can make the voice sound tight, strained, or breathy. In some people, the breaks occur once every few sentences. In more severe cases, spasms may occur on every word, making a person’s speech very difficult to understand. Some people with spasmodic dysphonia may also have vocal tremor—a shaking of the larynx and vocal folds that causes the voice to tremble.
Spasmodic dysphonia is a chronic condition that continues throughout a person’s life. Spasmodic dysphonia may develop suddenly, with severe voice symptoms present from the start of the disorder, or it may start with mild symptoms and occur only occasionally before worsening and becoming more frequent over time.
Spasmodic dysphonia is a rare disorder. It can affect anyone, but the first signs occur most often in people between the ages of 30 and 50. It affects more women than men.
What are the types of spasmodic dysphonia?
- Adductor spasmodic dysphonia is the most common form of spasmodic dysphonia. In this disorder, spasms cause the vocal folds to slam together and stiffen. These spasms make it difficult for the vocal folds to vibrate and produce sounds. The voice of someone with adductor spasmodic dysphonia may sound strained and strangled. The person’s speech may be choppy, with words cut off or difficult to start because of muscle spasms. The spasms are usually absent—and the voice sounds normal—while laughing, crying, or whispering. Stress often makes the muscle spasms more severe.
- Abductor spasmodic dysphonia is less common. In this disorder, spasms cause the vocal folds to remain open. The vocal folds cannot vibrate when they are open too far. The open position also allows air to escape from the lungs during speech. As a result, the voice often sounds weak and breathy. As with adductor spasmodic dysphonia, the spasms are often absent during activities such as laughing, crying, or whispering.
- Mixed spasmodic dysphonia, a combination of the above two types, is very rare. Because the muscles that open and the muscles that close the vocal folds are not working properly, it has features of both adductor and abductor spasmodic dysphonia.
What causes spasmodic dysphonia?
Spasmodic dysphonia is thought to be caused by abnormal functioning in an area of the brain called the basal ganglia. The basal ganglia help coordinate the movements of muscles throughout the body. Recent research has found abnormalities in other regions of the brain associated with spasmodic dysphonia, including areas of the cerebral cortex that control commands to muscles and coordinate these commands with incoming sensory information.
In some cases, spasmodic dysphonia may run in families. Although a specific gene for spasmodic dysphonia has not yet been identified, a mutation in a gene that causes other forms of dystonia has also been associated with spasmodic dysphonia.
How is spasmodic dysphonia diagnosed?
Diagnosis of spasmodic dysphonia can be difficult because the symptoms are often similar to those of other voice disorders. Diagnosis usually follows examination by a team, including:
- An otolaryngologist, a doctor who specializes in diseases of the ear, nose, throat, head, and neck. The otolaryngologist will pass a small lighted tube through the nose and into the back of the throat—a procedure called fiberoptic nasolaryngoscopy—to evaluate vocal fold anatomy and movements during speech and other activities of the larynx.
- A speech-language pathologist, a health professional trained to evaluate and treat voice, speech, and language disorders. The speech-language pathologist will assess voice symptoms.
- A neurologist, a doctor who specializes in nervous system disorders. The neurologist will evaluate for signs in the brain of dystonia and other movement disorders.
What treatment is available for spasmodic dysphonia?
There is currently no cure for spasmodic dysphonia, but treatment can help reduce its symptoms. The most common treatment is the injection of very small amounts of botulinum toxin directly into the affected muscles of the larynx. Botulinum toxin is produced by Clostridium botulinum, the same bacterium found in improperly canned foods and honey. The toxin weakens muscles by blocking the nerve impulse to the muscle. Botulinum toxin injections generally improve the voice for three to four months, after which voice symptoms slowly return. Reinjections are needed to maintain a good speaking voice. Initial side effects include a temporarily weak, breathy voice and occasional swallowing problems, but these usually improve after a few days to a few weeks. Botulinum toxin injections are more effective with adductor spasmodic dysphonia than with abductor spasmodic dysphonia. They do not help in every case.
Behavioral therapy (voice therapy) may reduce symptoms in mild cases. Voice therapy may work along with botulinum toxin injections to reduce voice strain. Some people may also benefit from psychological counseling to help them accept and live with their voice problems.
Augmentative and assistive devices can help some people with spasmodic dysphonia to communicate more easily. Some devices can help amplify a person’s voice, whether in person or over the phone. Computer software and tablet or smartphone apps can be used to translate text into synthetic speech.
When more conventional measures have failed, surgery may be performed on the larynx. Several surgical approaches are used to treat spasmodic dysphonia. Some surgical treatments show overall positive outcomes, but the results are not the same for all individuals. To date, there are no comparative studies pointing to a single, best treatment.
A physician can explain the potential outcomes, risks, and benefits of surgical treatment and can help to manage expectations.
What research does the NIDCD support on spasmodic dysphonia?
The National Institute on Deafness and Other Communication Disorders (NIDCD) currently funds research to better understand spasmodic dysphonia, determine its causes, and develop new diagnostics and better treatment options. NIDCD-supported scientists are conducting research to identify brain abnormalities and genes that cause spasmodic dysphonia. Through this research program, the NIDCD is directly addressing the need for more accurate detection, prediction, and diagnosis. NIDCD-funded scientists are also pursuing several new areas for future therapies and surgical interventions, including locating specific brain areas involved in regulating abnormal laryngeal muscle activity and looking for new oral medications that affect the abnormal brain activity underlying spasmodic dysphonia. Researchers are also working to determine if deficits in auditory and sensory feedback processing contribute to spasmodic dysphonia symptoms.
Visit the NIH Clinical Research Trials and You website to read about these and other clinical trials that are recruiting volunteers.
Where can I find more information on spasmodic dysphonia?
The NIDCD maintains a directory of organizations that provide information on the normal and disordered processes of hearing, balance, taste, smell, voice, speech, and language.
For more information, contact us at:
NIDCD Information Clearinghouse
1 Communication Avenue
Bethesda, MD 20892-3456
Toll-free voice: (800) 241-1044
Toll-free TTY: (800) 241-1055
Email: nidcdinfo@nidcd.nih.gov
NIH Publication No. 10-4214
March 2020
*Note: PDF files require a viewer such as the free Adobe Reader.

