On this page:
- Why is it important to have my baby’s hearing screened early?
- When will my baby’s hearing be screened?
- How will my baby’s hearing be screened?
- What should I do if my baby’s hearing screening reveals potential hearing loss?
- The follow-up exam revealed that my baby’s hearing is fine. Does that mean we don’t need to check his or her hearing again?
- How can I help my child with hearing loss develop language skills?
- What devices could help my child hear and communicate better?
- What language and communication approaches are available for my child?
- Will my child be successful in school?
- Baby’s hearing screening and next steps: Timeline for parents
- Where can I find more information about hearing screening and communication approaches?
Most children hear and listen to sounds at and even before birth. They learn to talk by imitating the sounds they hear around them and the voices of their parents and caregivers. But that’s not true for all children. In fact, about two or three out of every 1,000 children in the United States are born with detectable hearing loss in one or both ears. More lose hearing later during childhood. Children who have hearing loss may not learn speech and language as well as children who can hear. For this reason, it’s important to detect hearing loss as early as possible.
Because of the need for prompt identification of and intervention for childhood hearing loss, universal newborn hearing screening programs currently operate in all U.S. states and most U.S. territories. With help from the federal government, every state has established an Early Hearing Detection and Intervention Program. As a result, about 98% of babies have their hearing screened before 1 month of age.
Why is it important to have my baby’s hearing screened early?
The most important time for a child to learn language (spoken or signed) is in the first 3 years of life, when the brain is developing and maturing. In fact, children with typical hearing begin learning speech and language in the first 6 months of life. This is why it is so important to screen and start interventions for hearing loss as early as possible. Research shows that children with hearing loss who get help early develop better language skills than those who don’t.
When will my baby’s hearing be screened?
Your baby’s hearing should be screened before he or she leaves the hospital or birthing center. If not, make sure the baby is tested during the first month of life. If your baby’s hearing was not tested within 1 month of birth, or if you haven’t been told the results of the hearing screening, ask your child’s doctor today. Quick action will be important if the screening shows potential hearing loss.
How will my baby’s hearing be screened?
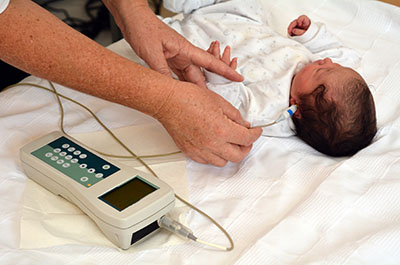
A newborn undergoes a hearing screening.
Two different tests are used to screen for hearing loss in babies. Your baby can rest or sleep during both tests.
- Otoacoustic emissions (OAE) tests whether some parts of the ear respond to sound. During this test, a soft earphone is inserted into your baby’s ear canal. It plays sounds and measures an "echo" response that occurs in ears with normal hearing. If there is no echo, your baby might have hearing loss.
- The auditory brain stem response (ABR) tests how the auditory nerve and brain stem (which carry sound from the ear to the brain) respond to sound. During this test, your baby wears small earphones and has electrodes painlessly placed on his or her head. The electrodes adhere and come off like stickers and should not cause discomfort.
What should I do if my baby’s hearing screening reveals potential hearing loss?
If the results show that your baby may have hearing loss, make an appointment with a pediatric audiologist—a hearing expert who specializes in the assessment and management of children with hearing loss. This follow-up exam should be done as soon as possible, ideally by the time the baby is 2 to 3 months old. The audiologist will conduct tests to determine whether your baby has a hearing problem and, if so, the type and extent of that problem.
If you need help finding a pediatric audiologist, ask your pediatrician or the hospital staff who conducted your baby’s screening. They may even be able to help you schedule an appointment. You can also try the directories provided by the American Academy of Audiology or the American Speech–Language–Hearing Association. If the follow-up examination confirms that your baby has hearing loss, he or she should begin receiving intervention services as soon as possible, ideally by the age of 3 to 6 months. See our Baby’s hearing screening and next steps: Timeline for parents (below) for a guide to follow.
The pediatric audiologist may recommend that your baby visit a pediatric ear, nose, and throat (ENT) physician who specializes in conditions affecting the ear, known as a pediatric otologist. A pediatric otologist can determine possible causes of hearing loss and recommend intervention options. If your child has siblings, the audiologist or otologist may also recommend that their hearing be tested.
The follow-up exam revealed that my baby’s hearing is fine. Does that mean we don’t need to check his or her hearing again?
Not necessarily. Hearing loss can occur at any time of life. Some inherited forms of hearing loss don’t appear until a child is older. If your baby was exposed to certain infections before being born, they are more likely to have gradual hearing loss during childhood. Other factors, such as childhood illness, ear infection, head injury, certain medications, and loud noise are also linked to hearing loss in children. Use Your Baby’s Hearing and Communicative Development Checklist to monitor and track your child’s communication milestones through age 5. If you have concerns about your child’s hearing at any age, talk to your pediatrician right away.
How can I help my child with hearing loss develop language skills?
When interventions begin early, children with hearing loss can develop language skills that help them communicate freely and learn actively. The Individuals with Disabilities Education Act ensures that all children with disabilities have access to the services they need to get a good education. Your community may also offer additional services to help support your child.
Your baby’s health care team will help you find services and methods to overcome communication barriers. You may also be referred to a speech-language pathologist or a teacher who is experienced in working with children with hearing loss. Talk to and communicate with your child often and stay up-to-date with all health care appointments.
What devices could help my child hear and communicate better?
Depending on your baby’s hearing loss and communication needs, some of these devices and tools may help to maximize his or her communication skills.
- Hearing aids. Worn behind the ear, hearing aids help make sounds louder and clearer. Hearing aids can be used for different degrees of hearing loss in babies as young as 1 month. A pediatric audiologist who is experienced in treating infants and children can help you choose the best hearing aid and make sure that it fits securely and is properly adjusted. Read the NIDCD fact sheet Hearing Aids for more information.
Cochlear implants. If your child cannot benefit from a hearing aid, your doctor or audiologist may suggest a cochlear implant. This electronic device can provide a sense of sound to people who are profoundly deaf or hard-of-hearing. The device converts sounds into electrical signals and carries them past the nonworking part of the inner ear to the brain. Since 2020, cochlear implants have been FDA approved for surgical placement in children as young as 9 months.
With training, children with cochlear implants can learn to recognize sounds and understand speech. Studies have also shown that eligible children (as young as 9 months of age) who receive a cochlear implant early may develop spoken language skills at a rate comparable to children with normal hearing, and many succeed in mainstream classrooms. Some doctors now recommend the use of two cochlear implants, one for each ear. An audiologist or otolaryngologist who specializes in cochlear implants can help you decide if a cochlear implant is appropriate for your child. Read the NIDCD fact sheet Cochlear Implants for more information.
- Assistive devices. As your child grows, other devices may be useful. Some devices help children hear better in a classroom. Others amplify one-on-one conversations or make talking on the phone or watching TV and videos easier. Read the NIDCD fact sheet Assistive Devices for People with Hearing, Voice, Speech, or Language Disorders for more information.
What language and communication approaches might be available for my child?
Children who are deaf or hard-of-hearing can learn to communicate in several ways. Find out as much as you can about the communication choices and ask your health care team to refer you to experts if you want to know more. Because language development begins early, regardless of the communication mode you choose, you should engage with your child and begin intervention as soon as possible.
Common approaches used to help children with hearing loss communicate and interact with others include:
- Listening and spoken language (also known as auditory-verbal): works to strengthen listening, talking, and reading skills through the use of natural hearing and hearing devices such as hearing aids and cochlear implants, without the use of manual communication.
- Auditory-oral: emphasizes residual natural hearing in combination with amplification devices and technology to help children develop speech and spoken-language skills. It includes the use of speech reading and natural gestures in the communication process.
- Cued speech: is a system of specific hand shapes and placements that represent groups of consonants and vowels and that are used in combination with natural lip movements.
- American Sign Language: is a visual-manual, natural language that is used in the American Deaf community.
- Combined approaches: use aspects of various communication approaches, some of which are listed above, to expose children who are deaf or hard-of-hearing to many ways to communicate with others.
Will my child be successful in school?
Like all children, children who are deaf or hard-of-hearing can develop strong academic, social, and emotional skills and succeed in school. Find out how your school system helps children with hearing loss. With your input, your child’s school will develop an Individualized Education Program (IEP) or Individualized Family Service Plan (IFSP) for your child, and you should ask if an educational audiologist is available to be part of the academic team. Explore programs outside of school that may help you and your child and talk with other parents who have already dealt with these issues. The Individuals with Disabilities Education Act ensures that children with hearing loss receive free, appropriate, early-intervention services from birth through the school years. Contact the U.S. Department of Education, along with resources listed in our directory of organizations.

An educator teaching a young boy.
Baby’s hearing screening and next steps: Timeline for parents
Use this timeline to get started.
By 1 month old:
| Make sure that your baby’s hearing is screened either before you leave the hospital or immediately afterward. After the screening, find out the results. If your newborn was not screened in the hospital, schedule a screening to occur by the time your baby is 1 month old. |
By 2-3 months old:
| If your baby did not pass the hearing screening, immediately schedule a follow-up appointment with a pediatric audiologist. Ask your doctor or hospital for a list of pediatric audiologists, or use the directories provided by the American Academy of Audiology and the American Speech–Language–Hearing Association. | |
| If you must cancel the follow-up appointment, reschedule it! Make sure you take your baby to a follow-up examination. This can occur as early as 2 months after birth, and by age 3 months at the latest. |
By 3-6 months old:
| If the follow-up exam shows that your baby has hearing loss, start your baby in some form of intervention as soon as possible. Your baby can start receiving intervention services as early as 3 months after birth and no later than 6 months. Interventions can include hearing devices, such as hearing aids or cochlear implants, and various language and communication approaches. Ask your health care team about the options. |
Ongoing:
| Remain active and involved in your child’s progress. | |
| If you move or change your contact information, make sure to tell your child’s doctors and specialists. | |
| Even if the follow-up exam found no sign of hearing loss in your child, continue to monitor his or her communication development. If you have concerns, speak with your child’s doctor. If your child has risk factors for childhood hearing loss, speak with an audiologist about how often his or her hearing should be monitored. |
Where can I find more information about hearing screening and communication approaches?
NIDCD maintains a directory of organizations providing information on the normal and disordered processes of hearing, balance, taste, smell, voice, speech, and language.
For more information, contact us at:
NIDCD Information Clearinghouse
1 Communication Avenue
Bethesda, MD 20892-3456
Toll-free voice: (800) 241-1044
Toll-free TTY: (800) 241-1055
Email: nidcdinfo@nidcd.nih.gov
NIH Publication No. 21–4968
October 2021
*Note: PDF files require a viewer such as the free Adobe Reader.

